Understanding Peripheral Vascular Diseases
Peripheral vascular diseases (PVDs) are a range of disorders that affect the blood vessels outside the heart and brain. These conditions can significantly impact circulation, leading to discomfort, pain, and potential complications. Proper understanding, timely intervention, and expert care are vital in managing PVDs effectively.
Peripheral Vascular Diseases
Peripheral vascular diseases (PVDs) encompass various disorders affecting the intricate network of blood vessels outside the heart and brain. This includes the arteries, veins, and lymphatic vessels supplying the arms, legs, stomach, pelvis, and organs.
PVDs arise due to vessel damage, blockages, or compression that disrupt normal blood circulation. This can cause tissues to be deprived of vital oxygen and nutrients, swelling, and/or pain. PVDs can manifest with various symptoms ranging from mild to debilitating.
Catching PVDs early provides the best opportunity to stop disease progression and prevent catastrophic complications. Lifestyle changes, medications, or minimally invasive treatments can significantly reduce the detrimental effects of PVDs. Promoting public awareness and prompt specialist evaluation for emerging symptoms are vital steps in mitigating the systemic impact of peripheral vascular disease.
The Rising Impact of Peripheral Vascular Diseases
Peripheral vascular conditions (PVDs) are a growing problem in the United States. According to the American Heart Association, more than 20 million adults in the United States have peripheral artery disease (PAD), and more than 30 million adults have chronic venous insufficiency (CVI). Several factors contribute to the rising impact of PVDs. These factors include:
- The aging population
The number of people in the United States aged 65 and older is expected to more than double by 2060. As people age, they are more likely to develop PVDs. - Increased rates of obesity
Obesity is a significant risk factor for PVDs. The prevalence of obesity in the United States has more than doubled since 1980. - Increased rates of diabetes
Diabetes is another significant risk factor for PVDs. The prevalence of diabetes in the United States has more than quadrupled since 1980. - Smoking
Smoking is a significant risk factor for both PAD and CVI. The prevalence of smoking in the United States has declined in recent years, but it remains a significant public health problem.
When To See a Cardiovascular Specialist for Peripheral Vascular Diseases
When it comes to your vascular health, timely intervention is crucial to ensure the best possible outcomes. If you are experiencing any of the following symptoms or conditions related to peripheral vascular issues, it's essential to seek consultation with a cardiovascular specialist as soon as possible:
- Persistent Leg Discomfort
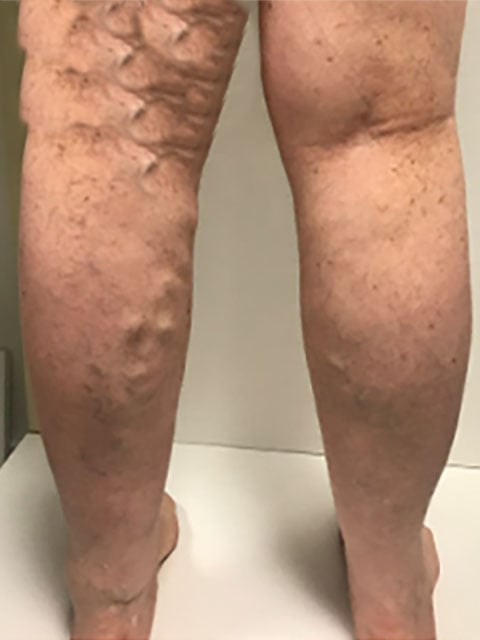
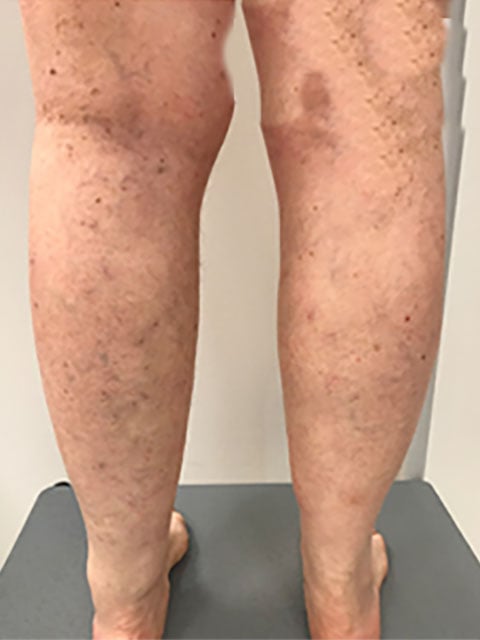
If you are consistently experiencing leg pain, cramping, numbness, or tingling, it could indicate an underlying vascular problem. Don't dismiss these symptoms as part of aging – they may require attention. - Visible Skin Changes
Skin discoloration, ulcers, or persistent wounds on your legs could be signs of vascular insufficiency or venous ulcers. Prompt assessment and treatment are important for reducing the risk of complications. - Swelling in the Legs or Feet
Unexplained swelling in your legs or feet may indicate poor circulation or other vascular issues. A cardiovascular specialist can diagnose the cause and recommend appropriate interventions. - Restless Legs or Leg Itching
If you are constantly experiencing the urge to move your legs or are troubled by itching or burning sensations, it's worth consulting a specialist to identify the underlying cause. - Aesthetic Concerns
If you have concerns about the appearance of your legs due to varicose veins, spider veins, or other vascular issues, a cardiovascular specialist can help address medical and cosmetic aspects. - Pelvic or Lower Back Discomfort
Pelvic pressure, lower back pain, and discomfort may be related to vascular issues such as venous congestion. Seeking evaluation can help determine the cause and appropriate treatment. - Non-Healing Wounds
If you have wounds on your legs that are not healing as expected, it could be due to compromised blood flow. Consulting a specialist can lead to effective wound management and improved vascular health. - Risk Factors
If you have risk factors for peripheral vascular diseases, such as a family history of vascular problems, smoking, diabetes, high blood pressure, or obesity, it's wise to seek regular assessments to catch issues early. - Decreased Mobility
If you notice a decrease in your ability to walk, exercise, or perform daily activities due to leg discomfort or pain, a specialist can help identify and manage the underlying cause.
Peripheral Vascular Diseases We Treat
Our experienced medical team is dedicated to providing comprehensive treatment for a wide range of peripheral vascular conditions. We specialize in diagnosing and managing various symptoms and disorders, including:
- Peripheral Arterial Disease (PAD)
PAD restricts blood flow to the legs, leading to symptoms like leg pain, cramping, and reduced mobility. Our interventions aim to improve circulation, alleviate discomfort, and prevent complications. - Deep Vein Thrombosis (DVT)
DVT is characterized by blood clots forming in deep veins, often in the legs. Our approach includes anticoagulation therapy and preventive measures to reduce the risk of complications like pulmonary embolism. - Chronic Venous Insufficiency (CVI)
CVI results from faulty leg veins, leading to swelling, pain, and skin changes. Our treatments aim to restore venous function, reduce discomfort, and enhance overall vascular health. - May-Thurner Syndrome
This condition occurs when a vein in the pelvis becomes compressed by an artery, leading to DVT. Our strategies focus on addressing the underlying compression and managing clot formation. - Pelvic Congestive Syndrome
Pelvic congestion causes chronic pelvic pain due to venous insufficiency. Our multidisciplinary approach targets the root cause, providing relief and improved quality of life. - Skin Changes / Discoloration
Discoloration, ulcers, and skin changes are indicative of underlying vascular issues. Our specialized care aims to address the vascular cause and promote healing. - Tingling in the Legs
Tingling sensations can arise from nerve compression or vascular issues. We conduct comprehensive evaluations to determine the source and deliver effective treatments. - Swelling in the Legs or Feet
Swelling can indicate venous insufficiency or lymphatic disorders. Our treatments focus on alleviating swelling and improving circulation. - Venous Ulcers
These open sores result from poor blood flow and can be painful. Our therapies promote healing, address underlying vascular issues, and prevent recurrence. - Wounds that Won't Heal
Non-healing wounds may stem from impaired circulation. Our approach addresses the vascular factors to enhance wound healing. - Restless Legs Syndrome (RLS)
RLS causes discomfort and an urge to move the legs, often due to circulatory issues. Our team addresses underlying causes and offers solutions to manage symptoms effectively. - Leg Itching / Burning / Numbness
These sensations can result from nerve or vascular problems. Our assessments help identify the source and guide appropriate treatments. - Aesthetic Appearance of Legs
We address cosmetic concerns stemming from vascular issues to help you achieve healthy and aesthetically pleasing legs. - Pelvic Pressure / Lower Back Pain
These symptoms may indicate venous congestion. Our treatments aim to alleviate pressure and discomfort by addressing underlying vascular issues.
Photo Gallery
Video Gallery
Testimonials
She made me feel like I was the most important person she could be taking care of.
Thanks to both of you it was a pleasant experience with absolutely no anxiety at all.
Dear Linda & Michelle: I wanted to thank you both for your excellent care given to me yesterday, when I was in your office for my PET scan. From the moment I arrived you explained everything to me in perfect detail so there were no “surprises” at all and I knew exactly what to expect. Kudos to you Linda for finding a vein for the IV right away! Michelle, you were very reassuring and by the way…you make good coffee!!!
I had my life back.
Doctor Dilip Viswanath made the recommendation that I start EECP therapy. I hugged the wall down the hall to my first session. I was able to walk back slow but without help. I felt better with each passing day. I had my life back. I have my freedom again and am able to drive again. I still have medical problems that are also being addressed but look at me now.
I felt as if I was the only one that mattered!
With the volume of people you serve, it would be so very easy to just “get them in and get them out,” but that was not the case. I felt as if I was the only one that mattered! So please extend my thanks and appreciation to your very excellent, professional and courteous staff.
My heart is full of thankfulness for how you took care of him.
Dear Dr. Rosenberg:
When B. turned twenty-one he was diagnosed with Lupus and he had his first heart attack. My thoughts at that time was that one day I might have to eulogize him despite all of my tears and prayers. For 53 years I lived with that dreaded thought but I was encouraged by your dutiful care of him. Your diligence and dedication to him personally was responsible for him reaching age 53.
You may not recall when you detected a totally blocked artery when he was in his late twenties. You consulted with Lupus specialists and heart surgeons to determine the next step. The surgeons were eager to perform because of B.'s blood clotting issues they would have to do a beating heart procedure, which according to them would mean a write up in medical journals. You pulled me aside to note that surgery would have a time limit and I quote: "No one is touching him until I am certain what is best for him because I intend to get him to a more normal longevity." Consequently, you gave him a stress test which indicated his body created its own natural bypass. I am sure that decision saved his life.
Not only did you minister to his medical difficulties and emergencies, you provided him with life-saving medications when his insurance carrier denied coverage. B. received the best care because you and your staff cared about him. Every complaint, discomfort and emergency was dealt with swiftly which gave us all a sense of comfort and relief. Amazingly, B. was afforded direct and personal contact with you. Who can call the doctor and be given direct access to him! B. could! I remember when he had an attack in Media, PA. I was with him when he contacted you. I spoke with you and indicated that I preferred that his hospitalization be in the Lady of Lords where you could take care of him. You immediately arranged for an ambulance. After heart attack number ten, surgery was required. While you were on vacation, you called daily to get updates on his condition following that quadruple bypass surgery.
My heart is full of thankfulness for how you took care of him. Your attention to his well-being gave me additional time to have him in my life. I cherished and admired him for he did not seek sympathy, nor did he bemoan his fate. He accomplished much in service to others. Despite pain or uncertainty, he answered all calls for help and mentored those in need. I firmly believe he is being rewarded for his good deeds and now he can finally rest. I miss him dearly and wish he had a longer life free of anxiety and pain.
Please extend my gratitude to your staff. Not only were they very kind and supportive toward him and in my presence hey spoke so highly of him and his dog. I am truly appreciative of their solicitude.
Photo Gallery
Meet Your [[CITY-LIST]]
Cardiovascular Physicians
In Search of Care? Request a Consultation Today
Please fill out the form below to explore your options for care and get your questions answered:

Your Cardiovascular Wellness Starts Now
Find a Cardiovascular Specialist Near You
Don't let peripheral vascular diseases affect your well-being. Our cardiovascular specialists are here to diagnose, treat, and manage these conditions to help you lead a healthier, more comfortable life. With several conveniently located office sites, you can access top-tier cardiovascular services close to home.

 Fax: 856-547-5337
Fax: 856-547-5337